Hand, Foot and Mouth Disease in Children: Symptoms, Home Care, EV71 Vaccine, When to See a Doctor
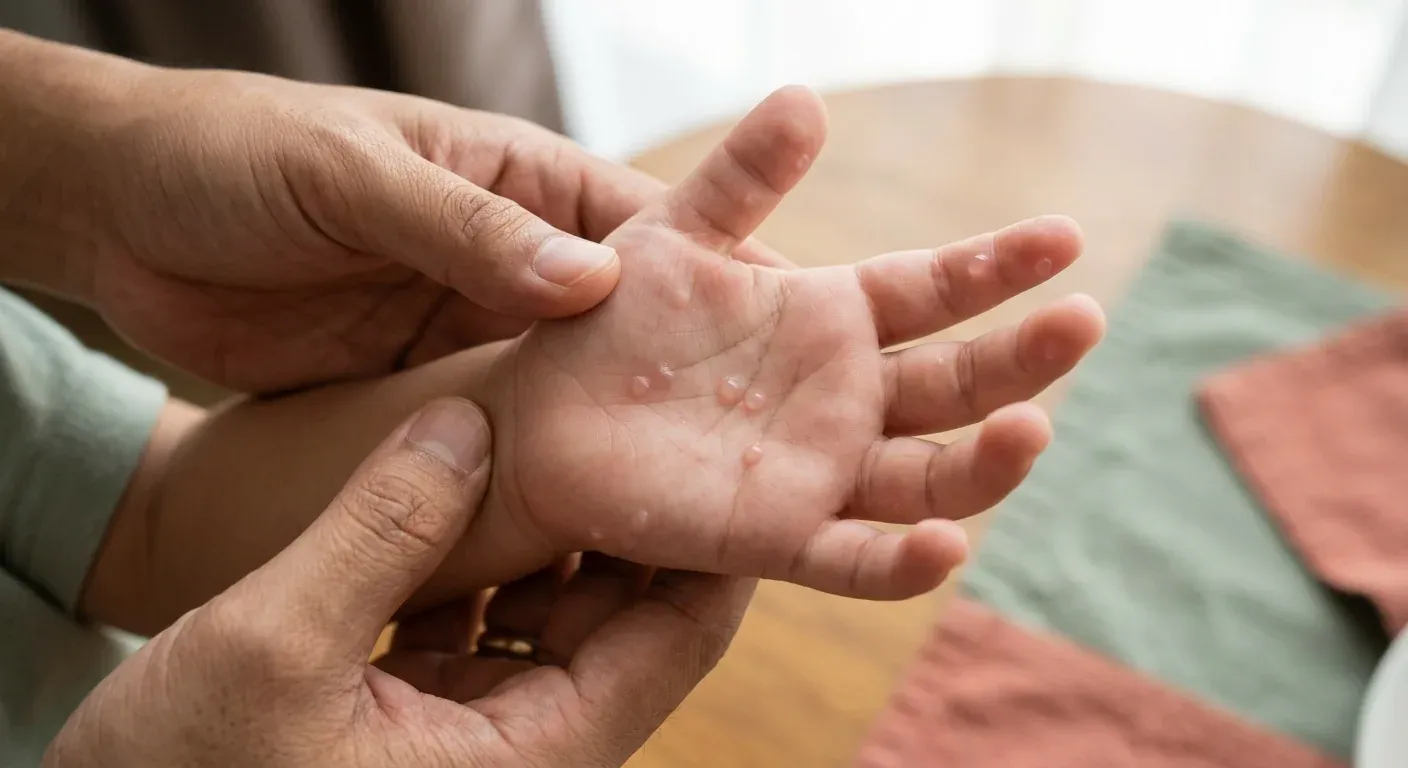
HFMD is common in young children during the rainy season — most cases clear in 7–10 days, but the EV71 strain can be life-threatening. AAP: "Symptoms are the worst in the first few days but are usually completely gone within a week."
Your toddler picks up hand, foot and mouth disease (HFMD) at nursery, then brings it home to a younger sibling — a scene Thai parents replay nearly every rainy season. This guide covers what to expect, how to care for your child at home, when to head straight to hospital, and what the EV71 vaccine does — drawn from NHS [1], AAP [2], CDC [3], Thailand's Department of Disease Control [4], and Samitivej Hospital [5][6].
NHS [1] sums it up:
"Hand, foot and mouth disease is a common childhood illness that can also affect adults. It usually gets better on its own in 7 to 10 days."
Most cases clear in 7–10 days — but the Enterovirus 71 (EV71) strain can cause severe brain and heart complications, and that's where parents need to know the warning signs.
What HFMD is
A common viral infection in children under 5, caused by viruses in the enterovirus family. Two strains matter most:
- Coxsackievirus A (especially A16) — the most common strain; symptoms are usually mild
- Enterovirus 71 (EV71) — less common, but can cause serious complications
AAP [2]:
"Hand, foot and mouth disease (HFMD) is a common viral illness in young children that typically spreads in summer and fall."
In Thailand, Samitivej [5] notes HFMD circulates year-round but rises during the rainy season (May–August) — a period the Department of Disease Control [4] tracks and issues advisories for every year.
Symptoms and progression
Incubation: 3–6 days
AAP [2] gives the timeline: after exposure, symptoms typically begin in 3–6 days.
Early symptoms (first 1–2 days)
Per AAP [2], the start looks like a common cold:
- Fever (often 38–39°C)
- Sore throat
- Runny nose
- Loss of appetite, fatigue
Later symptoms (days 2–4)
NHS [1] lists what comes next:
- Mouth ulcers — on tongue, gums, cheeks, palate; painful
- Rash and small blisters on hands, feet, sometimes the bottom, groin, or torso
- Spots may turn into blisters that are grey or lighter than surrounding skin
- Young children may drool more than usual because mouth sores make swallowing painful
Resolution in 7–10 days
CDC [3]: "Most children have mild symptoms for 7 to 10 days." Some children may have fingertip skin peeling 1–2 weeks later (AAP [2]).
How it spreads
CDC [3] calls HFMD "very contagious", with multiple transmission routes:
- Respiratory droplets from coughs, sneezes, talking
- Saliva, nasal secretions
- Fluid from blisters
- Stool — virus shedding in stool can continue long after recovery
- Toys and surfaces contaminated by any of the above
Most contagious window
NHS [1]:
"You can start spreading it from a few days before you have any symptoms, but you're most likely to spread it to others in the first 5 days after symptoms start."
But AAP [2] cautions that children can keep shedding virus in stool for weeks to months after they look better — which is why hand-washing after every diaper change matters even when the visible illness seems gone.
Home care
There's no specific antiviral for HFMD — care is supportive and lets the body clear the virus.
Prevent dehydration — the priority
Mouth ulcers make swallowing painful, so children stop drinking → dehydration risk.
NHS [1]:
"Drink cool fluids to soothe the mouth and prevent dehydration (but avoid acidic drinks, such as fruit juice)."
- Cool water soothes mouth ulcers
- Avoid acidic drinks (orange juice, pineapple juice) — the acid stings the ulcers
- Breastfed infants — keep nursing on demand, in shorter, more frequent sessions
Soft, cool, non-irritating foods
NHS [1]:
"Eat soft foods like yoghurt and avoid hot, salty and spicy foods."
- Yogurt, ice cream, cool milk, congee, soup — easy to swallow
- Avoid hot, spicy, salty, or crunchy foods
Fever and pain relief
- Paracetamol as advised by your pharmacist or pediatrician, dosed by weight
- Ibuprofen — for children 6 months and older
- No aspirin for children — CDC [3] warns explicitly
- No antibiotics — HFMD is viral; antibacterials don't help
Specific drug doses — ask your pharmacist or pediatrician. Don't calculate your own from internet sources.
Rest and hygiene
- Plenty of rest
- Trim nails short to prevent scratching blisters open and getting secondary infection
- Change diapers frequently and wash hands every time
Red flags — go to hospital immediately
Most cases stay mild and self-resolve — but EV71 can cause severe complications. Samitivej [5] lists what to watch for:
- Encephalitis (brain inflammation) — drowsiness, confusion, neck stiffness
- Myocarditis (heart muscle inflammation)
- Acute pulmonary edema — rapid, labored breathing
- Acute flaccid paralysis / muscle weakness
Go to hospital immediately if your child:
- Has persistent high fever (>39°C unresponsive to antipyretics) or fever for more than 3 days — AAP [2]: "Call your pediatrician if your child's fever lasts more than 3 days or if they are not drinking fluids."
- Becomes lethargic — hard to rouse, unresponsive
- Vomits repeatedly
- Has a seizure or jerky movements
- Has trembling hands, unsteady walking, frequent stumbling
- Shows rapid breathing, labored breathing, or pale skin
- Cannot drink or eat at all — dehydration signs (low urine output, dry mouth, no tears)
These signs may indicate EV71 affecting the brain, heart, or lungs — not symptoms to wait out at home.
School / nursery exclusion
NHS [1] gives advice based on how the child feels, not a fixed day count:
"Keep your child off school or nursery while they're feeling too unwell to go. But as soon as they're feeling better, they can go back to school or nursery. There's no need to wait until all the blisters have healed."
In short:
- Stay home while feverish, in pain, or unable to eat/drink
- Return when feeling better — don't wait for all blisters to clear
In the Thai context, Samitivej [5] suggests isolating for at least 5–7 days or until fully recovered — consistent with NHS [1]'s "first 5 days are most contagious" guidance.
Tip: If your child's school or nursery has a stricter return policy (waiting for all blisters to clear), follow the school's policy.
Prevention
No measure is 100% effective — especially for children in daycare — but you can cut the risk significantly.
Hand hygiene — the most important step
CDC [3] emphasises washing hands with soap and water for at least 20 seconds at these moments:
- After diaper changes
- Before preparing or eating food
- After using the toilet
- After returning from public places or daycare
Reduce household spread
- Don't share spoons, cups, toothbrushes, towels
- Clean toys, doorknobs, dining tables, and other frequently-touched surfaces
- With multiple children — separate personal items, limit close contact during illness
- Wash the patient's clothes and bedding on a hot wash
EV71 vaccine — a Thailand option
CDC [3] notes: "There is no vaccine in the United States to protect against the viruses that cause HFMD."
But in Thailand, an EV71 vaccine is available. Samitivej [6] summarises the basics:
- Age: 6 months to 5 years
- Doses: 2 injections, about 1 month apart
- Coverage: EV71 strain only — does not cover Coxsackievirus
- Benefit: Reduces the risk of severe complications (encephalitis, myocarditis, acute pulmonary edema)
The EV71 vaccine is an optional vaccine (not part of Thailand's routine MoPH schedule) — discuss with your pediatrician based on your child's risk, especially if they attend daycare.
Summary
- HFMD is caused by Coxsackie A and Enterovirus 71 — common in children under 5, peaks in rainy season
- Symptoms — fever, sore throat → mouth ulcers, blisters on hands and feet — most clear in 7–10 days
- Home care — prevent dehydration (cool fluids, yogurt, ice cream), paracetamol for fever, no aspirin, no antibiotics
- Hospital immediately if — persistent high fever, lethargy, repeated vomiting, seizures, trembling, unsteady walking, labored breathing, can't drink
- Stay home while unwell; return when feeling better (don't wait for blisters to clear)
- EV71 vaccine — Thailand option for children 6 months–5 years; reduces severe-complication risk from EV71 (does not cover Coxsackie)
Most cases of HFMD aren't dangerous — but knowing the EV71 red flags that need urgent care is the single most important thing to remember.
แหล่งอ้างอิง
- NHS — Hand, foot and mouth disease
- AAP HealthyChildren — Hand, Foot and Mouth Disease
- CDC — About Hand, Foot, and Mouth Disease
- Department of Disease Control, Thailand MoPH — Hand, Foot and Mouth Disease
- Samitivej Hospital — Hand, Foot and Mouth Disease (TH)
- Samitivej Hospital — EV71 Vaccine for HFMD (TH)